
Use of HQI’s updated Hospital Quality Improvement Platform (HQIP) — a quality analytics system that consolidates disparate data sources into a single, statewide platform — continues to increase as more hospitals complete their contract reviews.
The secure, web-based platform provides quality measures for conditions most affected by hospital quality initiatives. Through the platform, hospitals gain access to clinically rich, timely reports to help easily identify opportunities for improvement and areas for focus. It is free to all California Hospital Association (CHA) members, does not connect to your electronic health records system, and uses data hospitals already report to the California Department of Health Care Access and Information (HCAI), the National Healthcare Safety Network (NHSN), and the California Maternal Quality Care Collaborative.
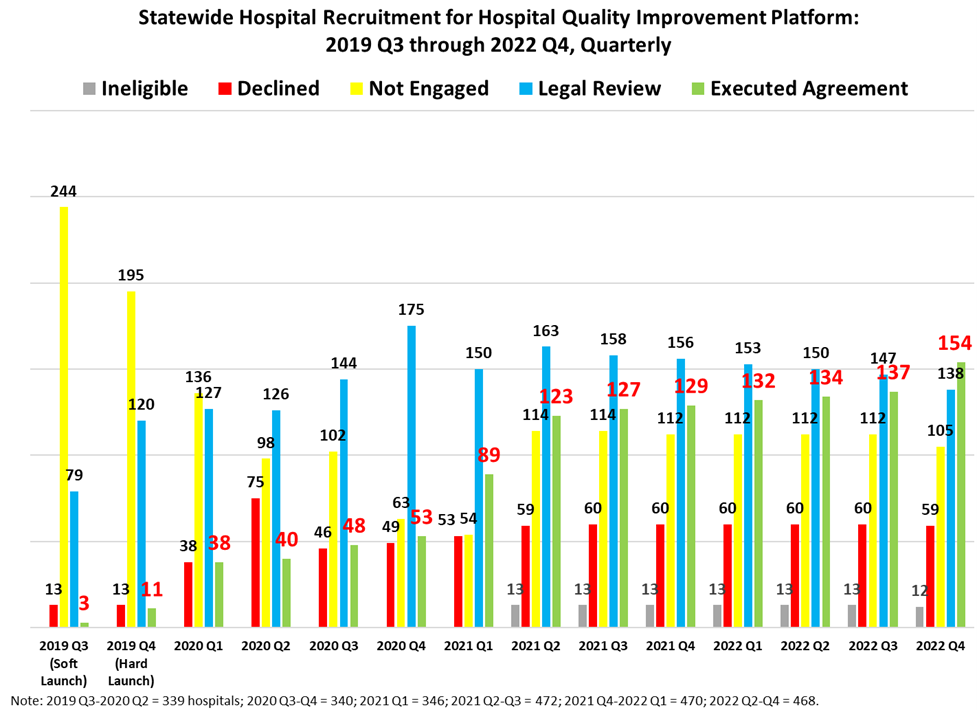
Since launching in October 2019:
- 339 of 468 hospitals have seen a demo of the platform.
- 154 hospitals have executed agreements.
- 138 hospitals have participation agreements under legal review.
NEW FEATURES AND UPDATES
- Loaded in 2021 statewide limited dataset (AB 2876)
- New “ED Encounter Type” filter allows users to include data for inpatient cases who were admitted from their emergency department (ED)
- Inpatient Encounter Reports are now grouped into modified diagnosis-related group (DRG) families instead of Clinical Classification Software Refined categories
- The comorbidity report classifications are now based on the Elixhauser Comorbidity Report methodology: Elixhauser Comorbidity Prevalence by Encounter Type
- Added Elixhauser Comorbidity Composite Index Rates & Trends Report
- Added Hospital-Acquired Condition Reduction Program Report
- New 2023 SIERA format functionality added to the upload dropdown options
- Added acuity level filter for ED reports
If you have input about features and measures you would like to see, email our HQI technical team at HQIAnalytics@hqinstitute.org.
WHAT’S TO COME IN FUTURE UPDATES
HQI is looking to improve various reports, such as readmission and mortality, by adding measures for diagnosis- and procedure-specific rates that track the definitions used by the Centers for Medicare & Medicaid Services for the Inpatient Quality Program. HQI is also developing new reports around severe maternal mortality, pediatric quality measures, disparities in quality outcomes, and rural hospital quality and reporting measures.
ABOUT THE PLATFORM
Features include:
- Access to hospital performance data from various sources, integrated into a centralized platform.
- Tools to understand your hospital’s quality performance and compare standardized measures to statewide benchmarks and peers.
- The ability to explore same-year quality performance for your hospital, rather than waiting eight to 20 months for statewide files to be released.
- An intuitive interface that provides a window into inpatient and emergency quality indicators.
- Secure data within HIPAA-qualified encrypted data systems.
Quality measures include:
- Inpatient case mix demographics, comorbidities, index
- ED discharge analytics (comorbidities, volume, demographics, revisits)
- Ambulatory surgery demographics
- Agency for Healthcare Research and Quality patient safety indicators
- Sepsis incidence and mortality
- Maternity measures
- Discharge volume by source (inpatient, ED, ambulatory surgery)
- Social determinants of health
- Chronic physical and behavioral conditions
- NHSN measures, trends, and details
There are 15 options for benchmarking your hospital’s performance:
- All CHA member hospitals
- Other critical access hospitals
- Other rural hospitals
- Other children’s hospitals
- Other teaching hospitals
- Other hospitals with the same payer (e.g., IEHP, PHC)
- Your hospital’s past performance
- Other CHA member hospitals:
- In the same health system
- In the same general region
- In the same health service area
- In the same metropolitan statistical area
- With similar bed size
- With the same type of control (e.g., non-profit)
- With the same license type
- With similar Medicare payer mix
- With similar Medi-Cal payer mix
- With the same adult/children’s trauma level designation
- With similar inpatient discharge volume
- With same ED service level (e.g., basic, standby)
- With similar outpatient visit volume
For hospitals interested in participating, it can be done in three easy steps:
- Execute the cost-free HQI-Hospital Service Agreement and HQI-Hospital Business Associated Agreement.
- Follow the HCAI Patient-Level Administrative Data (SIERA) HQIP Upload Instructions to securely submit copies of recent HCAI Patient-Level Administrative Data for ED, ambulatory surgery, and inpatient encounters.
- Follow our NHSN HQIP Group Join Instructions to confer rights to HQI’s NHSN group on the Centers for Disease Control and Prevention’s Secure Access Management Services web portal.
For more information about the HQIP or to schedule a 30-minute demo, visit the HQI website or email HQIAnalytics@HQInstitute.org.
